The staff provided excellent care, were nice to talk to and made a very comfortable visit. They were able to provide fillings to several chipped teeth with short notice while visiting Phoenix from out of country. Both myself and my dentist back home agreed the quality of the fillings were well done, and the colour was a great match. Highly recommend for the great staff and professional work done.
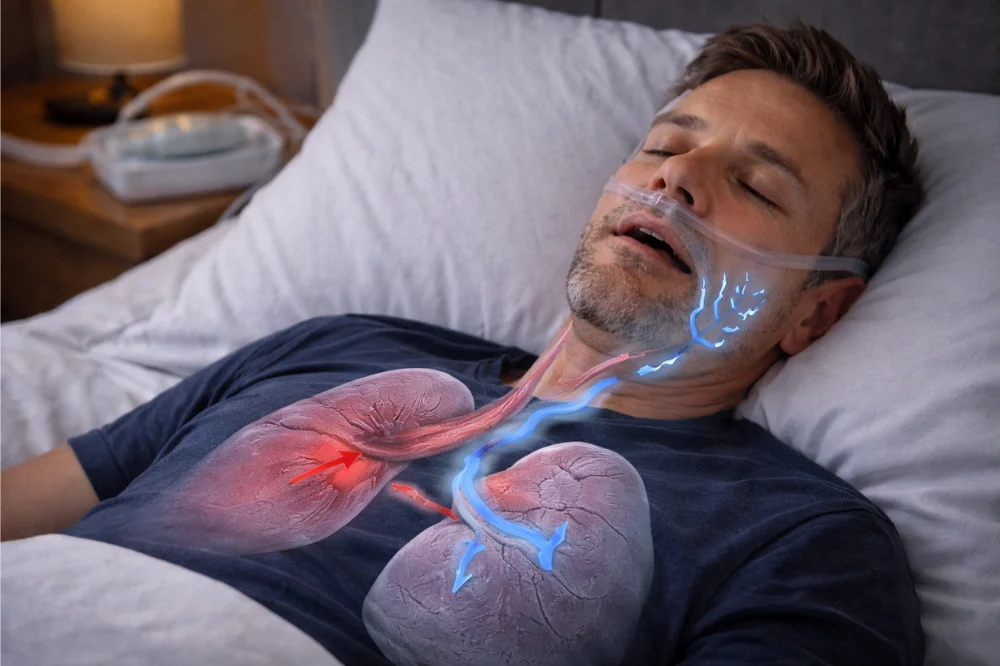
What causes sleep apnea is a question many adults ask after snoring, daytime exhaustion, or a new diagnosis. In simple terms, sleep apnea develops when breathing repeatedly stops or weakens during sleep, either because the airway collapses or the brain fails to signal steady breathing. Understanding the cause matters, because treatment works best when it targets why apnea is happening, not just the symptoms.
At Tempe Dentistry, Dr. Jeremy Chan helps patients uncover the underlying causes of sleep apnea as part of a broader airway and health evaluation. Dr. Chan earned his Doctor of Dental Surgery degree from the Arthur A. Dugoni School of Dentistry and completed his residency at El Rio Community Health Center. With advanced training in sleep-disordered breathing and TMJ disorders, and alignment with ADA, AADSM, and AASM guidelines, he focuses on cause-informed care that supports long-term health.
The Short Answer: What Actually Causes Sleep Apnea?
All sleep apnea comes down to one of two core problems that interrupt breathing during sleep. Either the airway physically narrows or collapses, or the brain does not send consistent signals to breathe. Everything else fits into one of these categories.
Obstructive sleep apnea, called OSA, happens when soft tissues or anatomy block airflow. Central sleep apnea, called CSA, occurs when the brain’s breathing control system becomes unstable. Some people experience a mix of both, known as complex sleep apnea.
A helpful way to think about this is simple. OSA is a plumbing problem involving airflow blockage. CSA is an electrical problem involving breathing signals. Most adults evaluated in Tempe dental and sleep clinics have OSA, but recognizing CSA is important for safety and proper treatment.
Structural Airway Causes: When Anatomy Narrows Breathing
For many adults, sleep apnea is driven by the physical shape of the airway. The size of the throat, tongue, jaw, and nasal passages all influence how easily air moves during sleep. Even people at a healthy weight can have significant airway narrowing.
Common structural contributors include a crowded throat, large tongue, long soft palate, or enlarged tonsils. Jaw structure also plays a major role. A small or retruded lower jaw, narrow upper jaw, high-arched palate, or crowded teeth can reduce space for the tongue and airway.
Nasal obstruction adds another layer. Chronic allergies, a deviated septum, or ongoing congestion force mouth breathing, which destabilizes the airway. In Tempe and the Phoenix area, seasonal allergies and dry desert air often worsen nasal inflammation, increasing risk for airway collapse.
Weight, Muscle Tone, and Lifestyle Factors
Weight and lifestyle strongly influence whether a borderline airway becomes obstructed. Excess weight is the single strongest risk factor for obstructive sleep apnea. Fat deposits around the neck, tongue, and throat physically compress the airway.
Muscle tone also matters. During sleep, throat muscles relax naturally. Alcohol, sedatives, and certain medications exaggerate this relaxation, making collapse more likely. Aging and hormonal changes, including perimenopause, further reduce muscle tone, especially in women.
Lifestyle habits compound risk. Smoking increases airway inflammation, while sleeping on the back allows the tongue to fall backward. In Tempe, hot weather often leads to indoor sedentary routines and evening alcohol use, which can quietly worsen airway stability.
Medical and Neurologic Causes: Central Sleep Apnea
Not all sleep apnea is caused by airway blockage. Central sleep apnea develops when the brain fails to maintain steady breathing signals during sleep. This type is less common but medically significant.
CSA is often linked to heart failure, stroke, neurologic disease, chronic opioid use, kidney failure, or high altitude exposure. Some people with heart failure develop a breathing pattern called Cheyne-Stokes respiration, marked by waxing and waning breaths.
Certain medications also contribute. Opioids and sedative-hypnotics can suppress respiratory drive. In mixed or complex cases, people have both airway collapse and unstable breathing control, requiring careful coordination of care.
Developmental, Genetic, and Sex-Related Factors
Many adults ask, “Why me?” even when they feel healthy. Genetics and early development often provide part of the answer. Family history of sleep apnea and inherited craniofacial traits can quietly shape airway size.
Childhood mouth breathing, allergies, enlarged tonsils, and orthodontic patterns influence jaw growth. Underdeveloped jaws and narrow dental arches are increasingly recognized as contributors to adult sleep apnea, even decades later.
Sex and age also matter. Sleep apnea is more common in men, but risk rises in women after menopause. Aging reduces muscle tone and worsens existing anatomical narrowing, increasing risk even without major weight gain.
Modifiable and Non-Modifiable Causes: What You Can Change
Some sleep apnea causes cannot be changed, while others can be improved with targeted action. Separating these helps set realistic expectations and reduces frustration.
The table below organizes common causes into those that are difficult to change and those that are modifiable or partially modifiable. This framework helps patients focus effort where it matters most.
| Cause Type | Examples | Change Potential | How It’s Addressed |
| Non-modifiable | Age, genetics, jaw shape | Limited | Airway therapies, appliances |
| Modifiable | Weight, alcohol, smoking | High | Lifestyle changes, support |
| Partially modifiable | Nasal obstruction, tonsils | Moderate | Medical or surgical care |
Understanding this breakdown helps patients avoid self-blame. It also reinforces that treatment often combines medical, dental, and lifestyle approaches.
From Cause to Treatment: How Your Profile Guides Care
Once the cause of sleep apnea is understood, treatment options become clearer. Different causes respond better to different therapies, which is why a one-size approach often fails.
Structural airway collapse may respond to CPAP, oral appliance therapy, airway-focused dental expansion, or ENT procedures. CSA related to heart or neurologic conditions requires management of the underlying disorder and specialized sleep therapies.
In Tempe, care often involves coordination. A typical path includes screening, a sleep study, cause analysis, and a tailored plan combining medical and dental solutions. Understanding cause improves comfort, adherence, and outcomes.
Taking the Next Step Toward Answers
Sleep apnea often leaves people stuck between worrying symptoms and unclear answers. You want to feel rested, healthy, and confident during the day, but confusion about what is causing the problem makes it hard to move forward. Understanding whether your sleep apnea comes from airway collapse, breathing signal issues, or a mix of factors is what turns uncertainty into a clear path.
Dr. Jeremy Chan’s role is to guide Tempe adults through that process with clarity and experience. He helps identify the real causes, explains the plan in plain language, and outlines next steps that make sense for your health and lifestyle. If you live near Downtown Tempe, South Tempe, or The Lakes, scheduling a consultation is how you move from ongoing frustration to informed action, with proper evaluation, appropriate sleep testing, and a treatment plan built around your specific needs
Frequently Asked Questions
Is sleep apnea always caused by being overweight?
This matters because many people blame weight alone and miss other contributors. A better question is whether anatomy, genetics, or medical conditions are involved. While weight is a major risk factor, many lean adults develop sleep apnea due to jaw structure, nasal obstruction, or neurologic causes.
What is the difference between obstructive and central sleep apnea?
This matters because treatment depends on the type. A better question is what mechanism is interrupting breathing. Obstructive apnea involves airway collapse, while central apnea involves unstable breathing signals from the brain.
Can dental issues really cause sleep apnea?
This matters because jaw and airway development are often overlooked. A better question is how jaw size and tongue space affect airflow. Narrow jaws, crowded teeth, and retruded jaws can significantly reduce airway space during sleep.
How do I find out what’s causing my sleep apnea?
This matters because guessing leads to ineffective treatment. A better question is how causes are evaluated properly. A sleep study combined with medical and dental airway assessment provides the most accurate picture.