The staff provided excellent care, were nice to talk to and made a very comfortable visit. They were able to provide fillings to several chipped teeth with short notice while visiting Phoenix from out of country. Both myself and my dentist back home agreed the quality of the fillings were well done, and the colour was a great match. Highly recommend for the great staff and professional work done.

TMJ treatment coverage can be confusing, and the short answer is that insurance coverage depends on the cause of your TMJ disorder and how treatment is classified. Some TMJ treatments may be covered by dental insurance, others by medical insurance, and many plans fall somewhere in between. Understanding this early helps patients avoid surprises and make informed decisions.
At Tempe Dentistry, Dr. Jeremy Chan helps patients sort through TMJ insurance questions with clarity and honesty. His background in TMJ disorders and dental sleep medicine allows him to explain not only what treatment is needed, but how it is typically billed and reviewed by insurance companies. This guidance helps patients focus on care first, not paperwork.
Why TMJ Insurance Coverage Is Often Complicated
TMJ disorder sits in a gray area between dental and medical care, which is where most insurance confusion begins. The jaw joint is part of the musculoskeletal system, yet dentists are often the providers diagnosing and treating TMJ problems. Because TMJ overlaps two systems, insurance companies do not always agree on how care should be categorized. This disagreement often leads to delays, partial coverage, or denied claims.
Insurance plans may classify TMJ treatment based on symptoms instead of how the jaw functions. Coverage decisions often depend on whether the issue is labeled as joint pain, muscle dysfunction, bite imbalance, or a dental concern. Understanding these classifications helps patients set realistic expectations before treatment starts. It also makes conversations with insurance providers more productive.
Dental Insurance and TMJ Treatment
Dental insurance sometimes covers parts of TMJ treatment, especially when care involves bite related concerns or oral appliances. This may include splints or devices designed to reduce clenching and support jaw position.
Coverage varies widely depending on the specific plan and how the treatment is coded. Even patients with similar insurance plans may see very different outcomes. Many dental plans place strict limits on TMJ benefits or exclude them altogether. Even when coverage exists, annual maximums, deductibles, and coinsurance often apply.
Patients are often surprised to learn that partial coverage does not always mean most of the cost is covered. Knowing this ahead of time helps avoid frustration.
Medical Insurance and TMJ Treatment
Medical insurance may cover TMJ treatment when the condition is linked to joint dysfunction, arthritis, or muscle disorders. This is more common when diagnostic imaging, referrals, or physical therapy are involved. In these cases, TMJ is treated as a medical joint condition rather than a dental issue. This distinction can make a difference in how claims are reviewed.
Medical plans often require detailed documentation and prior authorization before approving coverage. Claims may be denied if the treatment is considered dental in nature or if records are incomplete. Clear diagnosis and thorough documentation play a major role in whether medical coverage is approved. This is why evaluation and record keeping matter.
Factors That Influence Whether TMJ Treatment Is Covered
Insurance decisions are rarely based on a single detail. Several factors are reviewed together before coverage is approved or denied.
These factors help explain why two patients with similar symptoms may receive different coverage decisions. Understanding them early supports better planning.
Common factors include:
- How the TMJ disorder is classified as dental or medical
- The specific insurance plan and its exclusions
- Documentation showing pain or functional impairment
- The type of TMJ treatment recommended
Reviewing these factors ahead of time helps patients prepare financially and emotionally. It also reduces uncertainty before treatment begins.
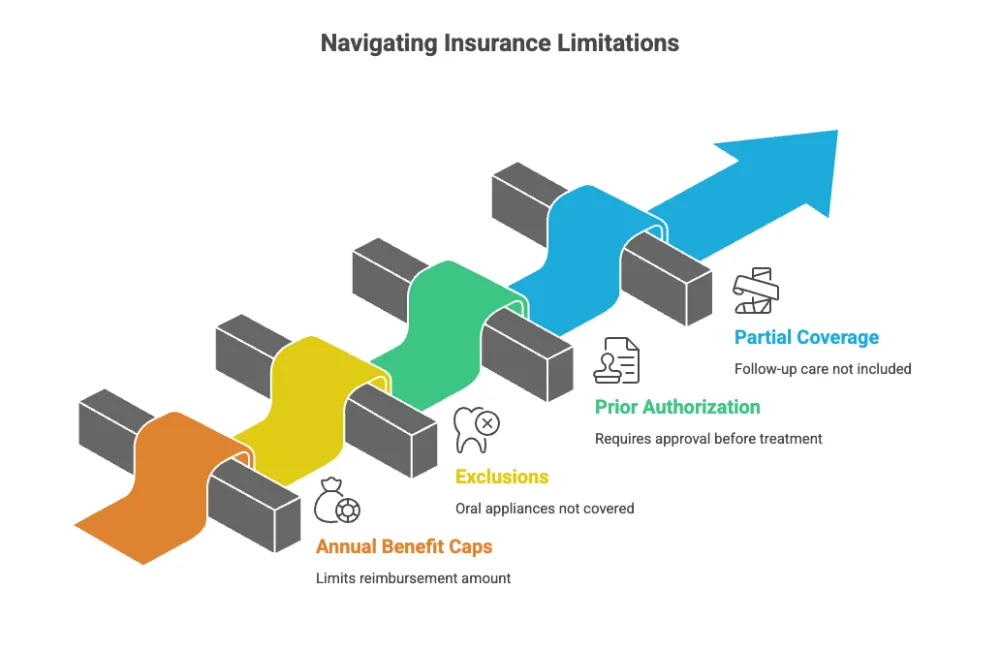
Common Limitations Patients Should Expect
Even when insurance provides some coverage, limitations are very common. These restrictions can apply to both dental and medical plans.
Knowing about these limits ahead of time allows patients to make informed decisions without feeling rushed.
Patients often encounter:
- Annual benefit caps that limit reimbursement
- Exclusions for oral appliances or splints
- Requirements for prior authorization
- Partial coverage that excludes follow up care
Understanding these limitations early prevents frustration later. It also helps patients plan for care more confidently.
How Dental and Medical Insurance Typically Differ for TMJ
Seeing insurance differences side by side often makes TMJ coverage easier to understand. A simple comparison can clarify why coverage outcomes vary.
The table below outlines how dental and medical insurance commonly approach TMJ treatment. This overview helps patients know what questions to ask.
| Coverage Type | What It May Cover | Common Limitations | What Patients Should Know |
| Dental Insurance | Oral appliances and bite related care | Low annual maximums and exclusions | Coverage is often limited or partial |
| Medical Insurance | Joint or muscle related treatment | Prior authorization and documentation | Approval depends on diagnosis and coding |
Understanding these differences helps patients feel more prepared when speaking with their insurance provider. It also supports clearer conversations with the dental team.
How Tempe Dentistry Helps With TMJ Insurance Questions
TMJ treatment decisions should never feel rushed or unclear. Dr. Jeremy Chan takes time to explain how recommended care is billed and what insurance may or may not cover.
This transparency helps patients feel informed before committing to treatment. Clear explanations build trust and reduce stress.
Patients from areas like South Tempe, The Lakes, and McClintock appreciate having these conversations upfront. Knowing insurance options early allows them to focus on improving comfort instead of worrying about unexpected costs.
Taking the Next Step With Confidence
Insurance questions can make TMJ treatment feel overwhelming, especially when pain is already affecting daily routines. Dr. Jeremy Chan serves as a guide for patients who want clarity rather than conflicting information.
Whether you live near Downtown Tempe, South Tempe, or The Lakes, the goal is the same, to understand your options and make informed choices. A consultation at Tempe Dentistry provides clarity about your TMJ condition, recommended treatment, and how insurance may apply to your care.
Frequently Asked Questions
Does dental insurance usually cover TMJ treatment?
This question matters because many patients assume dental insurance will automatically apply. That is not always the case.
What people should be asking instead is how their specific plan classifies TMJ care.
Some dental plans cover limited TMJ services, while others exclude them. Coverage depends on plan details and treatment type. Reviewing benefits early prevents surprises.
Sources: https://www.mouthhealthy.org/all-topics-a-z/tmj
Can medical insurance cover TMJ treatment?
Patients ask this when dental coverage is limited or denied. Understanding alternatives reduces stress.
A better question is when TMJ is considered a medical condition.
Medical insurance may cover TMJ treatment tied to joint or muscle disorders. Approval often requires documentation and prior authorization. Clear diagnosis improves outcomes.
Sources: https://www.nidcr.nih.gov/health-info/tmj
Why do insurance plans deny TMJ claims?
Denials feel frustrating and confusing. Knowing why helps patients respond appropriately.
A better question is how to reduce the risk of denial.
Claims are often denied due to classification issues or missing documentation. Proper diagnosis and clear records support coverage review.
Sources: https://www.mayoclinic.org
Should insurance decisions delay TMJ treatment?
Patients worry about timing and cost. This concern is understandable.
A better question is how to balance care needs with insurance realities.
Delaying care can allow symptoms to worsen. Many patients choose to move forward while exploring coverage options. A professional consultation helps guide this decision.
Sources: https://www.nidcr.nih.gov